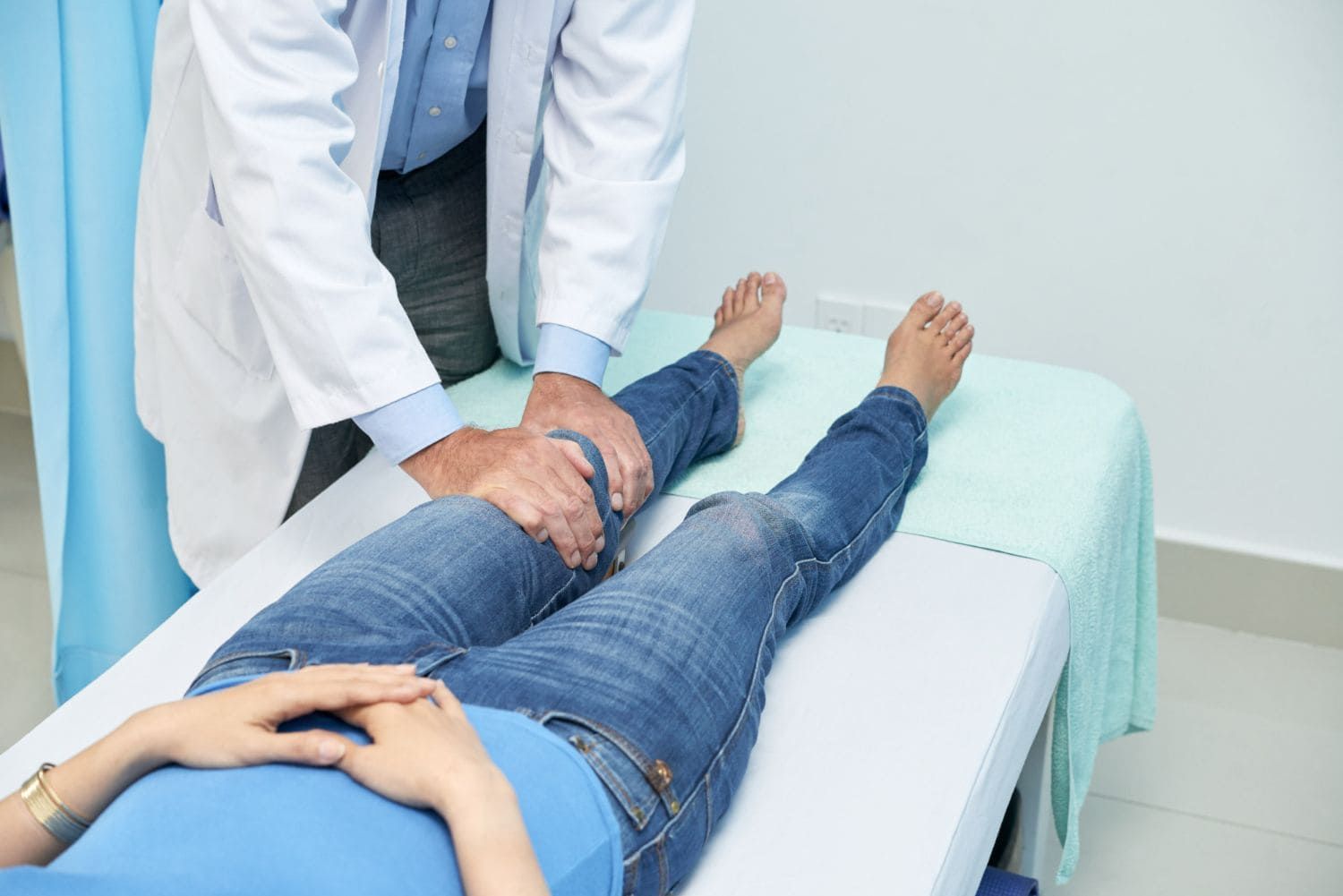
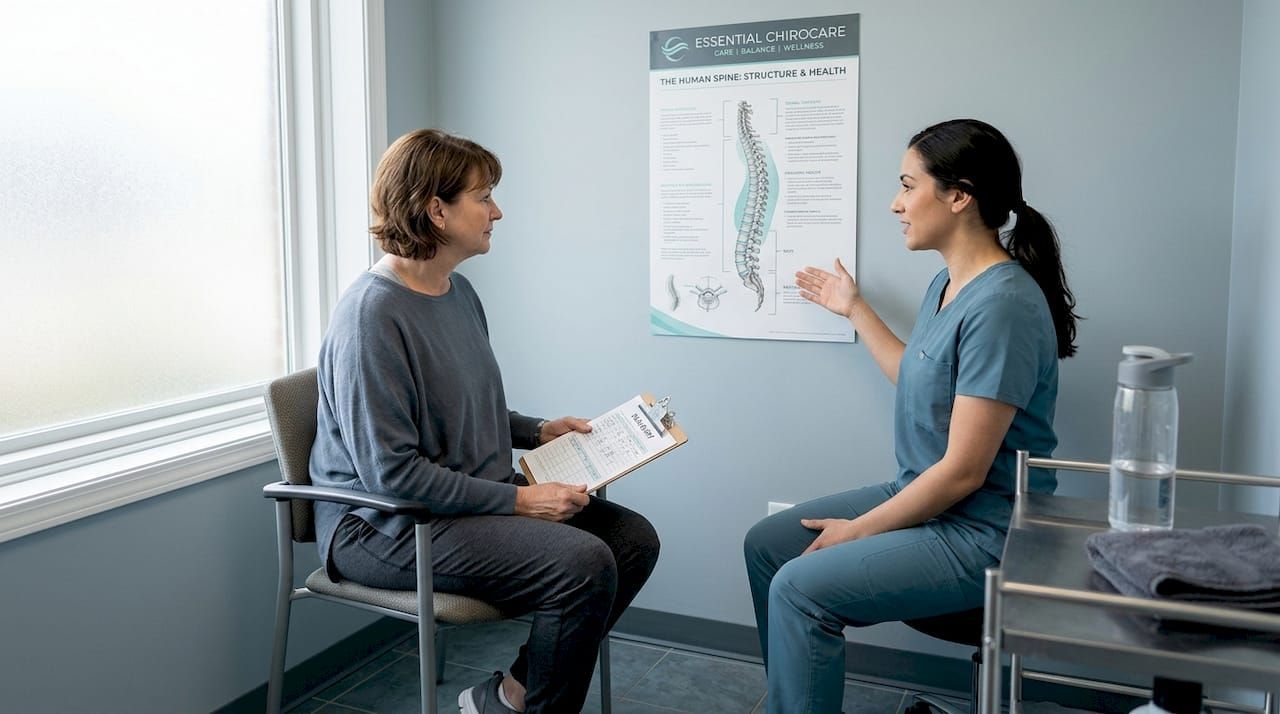
Early pain intervention: prevent chronic pain and boost wellness
Early pain intervention: prevent chronic pain and boost wellness
Most people assume that if they wait long enough, pain will simply fade. That assumption is costing them their health. Research now shows that 10 to 50% of people with acute pain transition to chronic pain when treatment is delayed. In West Central Florida, where active lifestyles and physical work are common, that risk is real and personal. This guide breaks down why acting fast on new pain is not an overreaction but a proven strategy for protecting your long-term wellness, avoiding opioid dependency, and getting back to the life you want.

Table of Contents
- Why early pain intervention matters
- Understanding the acute to chronic pain cycle
- The impact of early intervention: From science to real-world results
- Chiropractic care's role in early pain intervention
- Rethinking pain: Why early, personalized, and holistic care wins
- Holistic pain relief is closer than you think
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Act early | Prompt action helps prevent acute pain from becoming chronic with long-term consequences. |
| Holistic approach works | Combining chiropractic, psychosocial support, and exercise boosts pain outcomes. |
| Florida leads in solutions | West Central Florida's interdisciplinary programs show reduced costs and better pain relief. |
| Chiropractic is effective | Spinal manipulation and other chiropractic care match or outperform traditional pain solutions safely. |
Why early pain intervention matters
When pain first appears, your body is sending a clear signal. Ignore it, and that signal can become a permanent broadcast. Acute pain major risk for chronic pain if unmanaged is not just a clinical phrase. It describes what happens to real people who wait too long, hoping the discomfort will disappear on its own.
The numbers are stark. Studies consistently show that between 10% and 50% of individuals experiencing acute pain go on to develop chronic pain conditions. That range depends on factors like injury type, psychological state, and how quickly care begins. What stays constant is this: the longer pain goes unmanaged, the harder it becomes to treat.
"Inadequately managed acute pain is a major risk factor for chronic postsurgical pain and persistent opioid use." This finding underscores why early, structured care is not optional but essential for anyone serious about their recovery.
One of the most critical mechanisms behind this transition is central sensitization , a process where your nervous system becomes hypersensitive to pain signals. Think of it like a car alarm that keeps going off even after the threat is gone. Once central sensitization sets in, even mild stimuli can trigger significant pain responses, making everyday activities feel unbearable.
Psychosocial factors also accelerate this shift. Stress, anxiety, poor sleep, and social isolation all increase the likelihood that acute pain will become chronic. These are not soft concerns. They are measurable risk factors with biological consequences.
| Factor | Low-risk outcome | High-risk outcome |
|---|---|---|
| Time to treatment | Within 1 week | More than 4 weeks |
| Psychological state | Stable, supported | Anxious, isolated |
| Pain management approach | Multimodal, holistic | Wait-and-see, passive |
| Opioid use | Avoided or minimal | Prolonged reliance |
For residents across Tampa, Brandon, Sarasota, Lakeland, and Pinellas Park, getting acute pain relief early is not just about comfort. It is about preventing a cascade of physical and psychological consequences that become exponentially harder to reverse.
Understanding the acute to chronic pain cycle
Pain does not become chronic overnight. It follows a predictable pathway that science has mapped with increasing precision. Understanding that pathway gives you the power to interrupt it.
At the biological level, untreated pain triggers neuroinflammation , a process where immune cells in the nervous system release chemicals that amplify pain signals. Over time, this rewires how your brain processes pain, making it more sensitive and less accurate. Psychosocial factors in pain chronicity like depression and catastrophizing accelerate these neurological changes through epigenetic mechanisms, meaning your very gene expression can shift in response to prolonged pain and stress.
At the psychological level, catastrophizing (the tendency to expect the worst outcome from pain) and fear avoidance (avoiding movement because you fear making pain worse) are two of the strongest predictors of chronic pain. Both create a vicious cycle: less movement leads to more stiffness and weakness, which leads to more pain, which reinforces fear.
Common predictors that increase the risk of acute pain becoming chronic include:
- A history of depression or anxiety
- Previous trauma or injury in the same area
- Lack of social or family support
- High-stress work or home environments
- Sleep disturbances lasting more than two weeks
- Low confidence in recovery
The good news is that this cycle is interruptible. Early holistic care that addresses both physical and emotional components can stop neuroinflammation before it becomes entrenched. Chiropractic techniques that restore movement and reduce mechanical stress on the nervous system play a direct role in disrupting this cycle at the source.
Pro Tip: If you notice that your mood is worsening alongside your physical pain, mention it to your provider. Emotional health is not separate from pain recovery. Treating both together dramatically improves outcomes and shortens recovery time.
The impact of early intervention: From science to real-world results
Knowing the risks is useful. Seeing what happens when those risks are actively managed is even more compelling.
In West Central Florida, interdisciplinary pain management in Florida that includes chiropractic care has been formally recommended as a strategy to reduce costs and improve outcomes for state employees dealing with chronic pain. This is not a fringe suggestion. It reflects a growing recognition that early, coordinated care saves money and lives.
Research tracking local pain assessment progress shows measurable reductions in emergency room visits and hospitalizations when patients receive structured early intervention rather than reactive treatment.
| Outcome | Early intervention | Delayed intervention |
|---|---|---|
| Average recovery time | 4 to 6 weeks | 3 to 6 months |
| Opioid prescription rate | Significantly lower | Up to 3x higher |
| Total treatment cost | Reduced by up to 40% | Substantially higher |
| Risk of chronic pain | Minimized | Up to 50% transition rate |
Local clinics that prioritize holistic pain management typically follow a structured early-intervention process:
- Comprehensive initial assessment covering physical, neurological, and psychosocial factors
- Immediate mobilization and movement-based therapy to prevent deconditioning
- Patient education on pain science to reduce fear and catastrophizing
- Coordinated care with physical rehabilitation and manual therapy specialists
- Regular progress tracking with adjustments to the treatment plan based on response
This approach is not complicated. It is consistent, personalized, and grounded in evidence. The difference between a six-week recovery and a six-month struggle often comes down to whether steps like these were taken in the first week.

Chiropractic care's role in early pain intervention
Chiropractic care is often misunderstood as a last resort or an alternative to real medicine. The evidence tells a very different story.
Spinal manipulative therapy (SMT) , the core technique used by chiropractors, involves controlled force applied to specific spinal joints to restore movement and reduce nerve irritation. SMT effective for back and neck pain with cost-effectiveness ratios well below the $50,000 per quality-adjusted life year threshold used to evaluate medical interventions. For chronic low back pain, SMT performs comparably to exercise therapy and non-steroidal anti-inflammatory drugs, without the side effects.
A study on SMT confirms these findings across a broad patient population, reinforcing that chiropractic is a clinically sound choice for early pain intervention.
Key benefits of including chiropractic in your early care plan:
- Reduces central sensitization by restoring normal joint mechanics and nervous system signaling
- Improves range of motion quickly, allowing patients to stay active during recovery
- Lowers the need for opioid prescriptions, reducing dependency risk
- Cost-effective compared to surgical or long-term pharmaceutical approaches
- Can be integrated with physical rehabilitation, massage, and lifestyle coaching
Skeptics sometimes point to mixed results in placebo-controlled chiropractic studies. That nuance is worth acknowledging. SMT is not a universal cure, and outcomes vary by condition, patient profile, and provider skill. What the evidence consistently supports is that for the right patient at the right time, chiropractic care is among the most effective and safest early interventions available.
Explore chiropractic methods for chronic pain and the broader benefits of chiropractic pain management to understand how these approaches fit into a complete wellness strategy.
Pro Tip: Patients who begin chiropractic care within the first two weeks of an acute injury consistently report faster recovery and lower rates of pain recurrence. Early access is not a luxury. It is a clinical advantage.
Rethinking pain: Why early, personalized, and holistic care wins
Here is the uncomfortable truth most people are not told: the "wait and see" approach is not neutral. It is a choice with consequences. Every week of unmanaged pain is a week your nervous system spends learning to amplify that pain. That is not pessimism. That is neuroscience.
What we have seen working with patients across West Central Florida is that those who act early, even before pain becomes severe, recover faster, spend less, and rarely return with the same problem. The ones who wait often come back months later with a far more complex picture that requires longer, more intensive care.
Personalized care matters enormously here. Two people with the same back injury can have completely different recovery trajectories based on their stress levels, sleep quality, and support systems. A one-size-fits-all treatment plan misses this reality entirely.
The most effective approach combines spinal care with psychosocial support, patient education, and movement therapy. That combination is not radical. It reflects what the best chiropractic treatments research consistently recommends. The shift we are advocating for is simple: treat pain as urgent from day one, not as something to endure until it becomes a crisis.
Holistic pain relief is closer than you think
You now understand why acting early on pain is one of the most important health decisions you can make. The science is clear, the local evidence is strong, and the tools exist to help you recover fully without relying on medications or waiting for things to get worse.
At Essential ChiroCare, our experienced doctors provide expert pain relief through personalized, evidence-based chiropractic care across Tampa, Brandon, Sarasota, Lakeland, and Pinellas Park. Whether you are dealing with a new injury or a recurring problem, we build treatment plans around your specific needs and goals. Do not wait for acute pain to become a chronic condition. Relieve pain effectively by booking a consultation with our team today and taking the first real step toward lasting wellness.
Frequently asked questions
How soon should I seek care after new pain starts?
You should seek evaluation within the first few days of new pain, since early intervention drastically reduces the chance of acute pain becoming a chronic condition.
What makes chiropractic care suitable for early intervention?
Chiropractic care offers non-opioid pain relief and improved mobility, and SMT for neck and back can be combined with exercise and education for faster, more durable recovery outcomes.
Can psychological factors really increase my pain risk?
Yes, conditions like stress, depression, and catastrophizing predict pain chronicity through neuroinflammatory and epigenetic mechanisms, so addressing them early alongside physical treatment is essential.
Is waiting to see if pain improves ever safe?
Waiting increases your risk for chronic pain significantly, and early assessment provides more treatment options while lowering the risk of long-term complications and opioid dependence.
Recommended