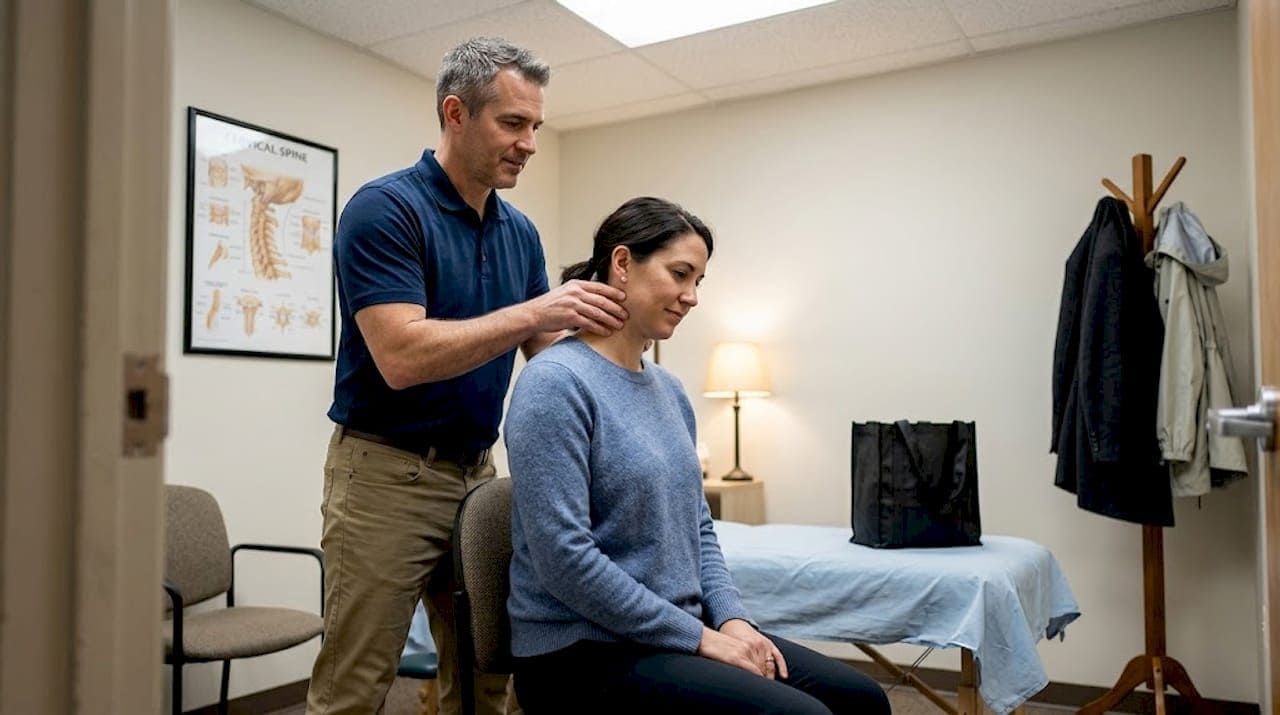
Streamline your injury recovery workflow for faster healing
Streamline your injury recovery workflow for faster healing
TL;DR:
- A structured injury recovery workflow provides a clear, step-by-step path from assessment to lasting results.
- Personalization, progress tracking, and ongoing evaluation are essential for effective rehabilitation.
- Consistent participation and long-term habits prevent reinjury and enhance full recovery.
You just got hurt, and now everyone has an opinion. Your neighbor says rest completely. Your coworker swears by ice baths. Your doctor mentioned physical therapy, but your insurance situation is a mess. Meanwhile, your pain is real, your function is limited, and you have no clear map for what comes next. This kind of confusion is exactly why so many people in West Central Florida end up stuck in a cycle of partial recovery, recurring pain, and frustration. A structured injury recovery workflow cuts through the noise and gives you a clear, step-by-step path from your first evaluation all the way to lasting results, with every decision based on your specific body and goals.

Table of Contents
- What is an injury recovery workflow?
- Step 1: Initial assessment and setting recovery goals
- Step 2: Customized treatment planning and execution
- Step 3: Monitoring progress and adjusting treatment
- Step 4: Achieving lasting results and preventing reinjury
- Why most people underestimate the power of a structured recovery workflow
- Take the next step in your recovery with expert help
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Personalized workflow matters | Tailored injury recovery plans yield better results than generic protocols. |
| Regular progress checks | Monitoring and adapting your plan ensures effective healing and prevents setbacks. |
| Integrated care advantages | Combining chiropractic, rehab, and lifestyle management creates lasting recovery. |
| Prevention is part of recovery | A good workflow teaches habits that help prevent future injuries. |
What is an injury recovery workflow?
In a medical or chiropractic context, a "workflow" is simply an ordered set of steps that guides your care from start to finish. Think of it like a GPS for your recovery: instead of guessing which turn to take, you follow a proven route that adapts when conditions change. The injury rehab process works the same way, moving through defined stages so nothing important gets skipped.
A step-by-step healing process matters because it creates accountability. When your care is organized, your provider can track what is working, spot problems early, and adjust before small setbacks become major ones. Without structure, it is easy to stop care the moment pain fades, which is often too early to prevent reinjury.
Here is how a typical workflow breaks down:
| Stage | What happens | Goal |
|---|---|---|
| Assessment | Injury history, pain mapping, function testing | Understand the full picture |
| Personalized plan | Goal-setting, treatment selection | Match care to your needs |
| Treatment | Adjustments, therapy, exercises | Reduce pain, restore function |
| Progress checks | Reassessment, plan updates | Confirm healing, catch setbacks |
| Return to activity | Gradual reintroduction, prevention | Sustain results long-term |
Personalized assessments and tracking improve adherence and outcomes over generic approaches. Here is why following this kind of structure works so well:
- You always know what phase you are in and what comes next
- Your provider can measure real improvement instead of guessing
- You avoid the "I feel fine, so I'll stop" trap that leads to relapse
- Every treatment decision is tied to a specific goal
- You build confidence as you hit measurable milestones
Step 1: Initial assessment and setting recovery goals
Understanding the workflow's outline, let's dive into how the process begins with assessment and goal-setting.
Your first visit sets the tone for everything that follows. A thorough evaluation is not just paperwork. It is the data-gathering phase that makes personalization possible. Personalization via assessments and progress tracking ensures tailored care, improving adherence and outcomes over generic protocols. Here is what a complete initial assessment typically covers:
- Injury and medical history review: Your provider asks about the mechanism of injury, how long you have had symptoms, and any previous injuries that might complicate healing.
- Pain mapping: You describe where it hurts, what makes it worse, and what provides temporary relief. This helps identify referred pain patterns and nerve involvement.
- Postural and structural evaluation: Your provider looks at how you stand, walk, and move to find compensations your body has developed around the injury.
- Orthopedic and neurological testing: Specific tests check joint integrity, muscle strength, and nerve function to rule out serious pathology.
- Goal-setting conversation: You and your clinician agree on realistic, measurable milestones, like returning to your morning run or getting through a workday without pain.
This last step is often skipped in rushed care settings, and that is a mistake. When goals are specific and personal, you stay motivated and your provider knows exactly what success looks like for you. Restoring function safely is the guiding principle here, not just chasing pain relief.
Pro Tip: Before your first appointment, write down your three most limiting symptoms, when they started, and what activities you can no longer do. This simple list can cut your assessment time in half and help your provider zero in on what matters most.
Step 2: Customized treatment planning and execution
With goals now set, the next stage is crafting and following through on a plan tailored to your needs.
A generic treatment plan treats every patient the same. A personalized one treats you. Clinics in Tampa, Clearwater, and Hillsborough County offer integrated non-surgical care for injuries from various causes, and the key word there is integrated. Combining multiple treatment approaches produces better results than any single therapy alone.
Here are the major treatment types and what each one brings to your recovery:
- Chiropractic adjustments: Restore proper joint alignment, reduce nerve irritation, and improve range of motion. Most patients notice reduced pain and better mobility within the first few sessions.
- Manual therapy: Soft tissue work like myofascial release breaks up scar tissue, reduces muscle tension, and improves circulation to injured areas.
- Physical rehabilitation: Targeted exercises rebuild strength and stability in the muscles surrounding an injured joint, reducing the chance of reinjury.
- Spinal decompression: Particularly effective for disc-related injuries, this therapy gently stretches the spine to relieve pressure on compressed nerves.
- Home exercise programs: What you do between visits matters just as much as what happens in the clinic. Consistent daily movement accelerates healing.
- Nutrition support: Recovery nutrition tips show that anti-inflammatory foods and adequate protein directly speed tissue repair.
Here is how a standard plan compares to a personalized one:
| Feature | Standard plan | Personalized plan |
|---|---|---|
| Treatment selection | Same for all patients | Based on your specific injury and goals |
| Progress benchmarks | Fixed timeline | Adjusted to your rate of healing |
- Nutrition guidance | Rarely included | Integrated when relevant | | Home exercises | Generic handout | Tailored to your limitations | | Communication | Scheduled only | Ongoing, responsive to changes |
For athletes and active individuals, recovery approaches for sports injuries and top chiropractic techniques can be layered into the plan to address performance demands alongside pain relief.
Pro Tip: Consistency beats intensity every time. Showing up for three moderate sessions per week produces better results than one aggressive session followed by days of rest. Your nervous system and connective tissue heal through repetition, not heroics.
Step 3: Monitoring progress and adjusting treatment
Once your treatment is underway, ongoing evaluation is essential to ensure progress and prevent setbacks.
This is where many recovery plans quietly fall apart. Patients start feeling better, skip a check-in, and then wonder why they plateau or regress. Personalization via progress tracking leads to improved adherence and outcomes, and that is not an accident. Tracking creates a feedback loop that keeps your care sharp. Here is how to do it well:
- Rate your pain daily on a 1 to 10 scale and note what triggered any changes. Patterns reveal what is helping and what is not.
- Track your functional gains. Can you bend further? Sleep through the night? Walk without limping? These markers matter more than pain scores alone.
- Log your home exercises with notes on how your body responded. This gives your provider real data to work with at each visit.
- Communicate flare-ups immediately. Do not wait for your next appointment if something feels significantly worse. A quick call or message can prevent a minor setback from becoming a major one.
Your provider will use this information to decide whether to advance your program, switch therapies, or address a new symptom. Athlete recovery tips emphasize the same principle: adaptation is the engine of progress. Strategies like mindfulness for recovery setbacks can also help when stress or anxiety is slowing your physical healing.
"Missing check-ins can slow your healing, even if you feel better."
This is one of the most important truths in injury recovery. Pain reduction is not the finish line. It is a milestone on the way to full function. Ending care early because you feel okay is like leaving a construction site before the foundation is finished. The structure looks fine until the first storm.
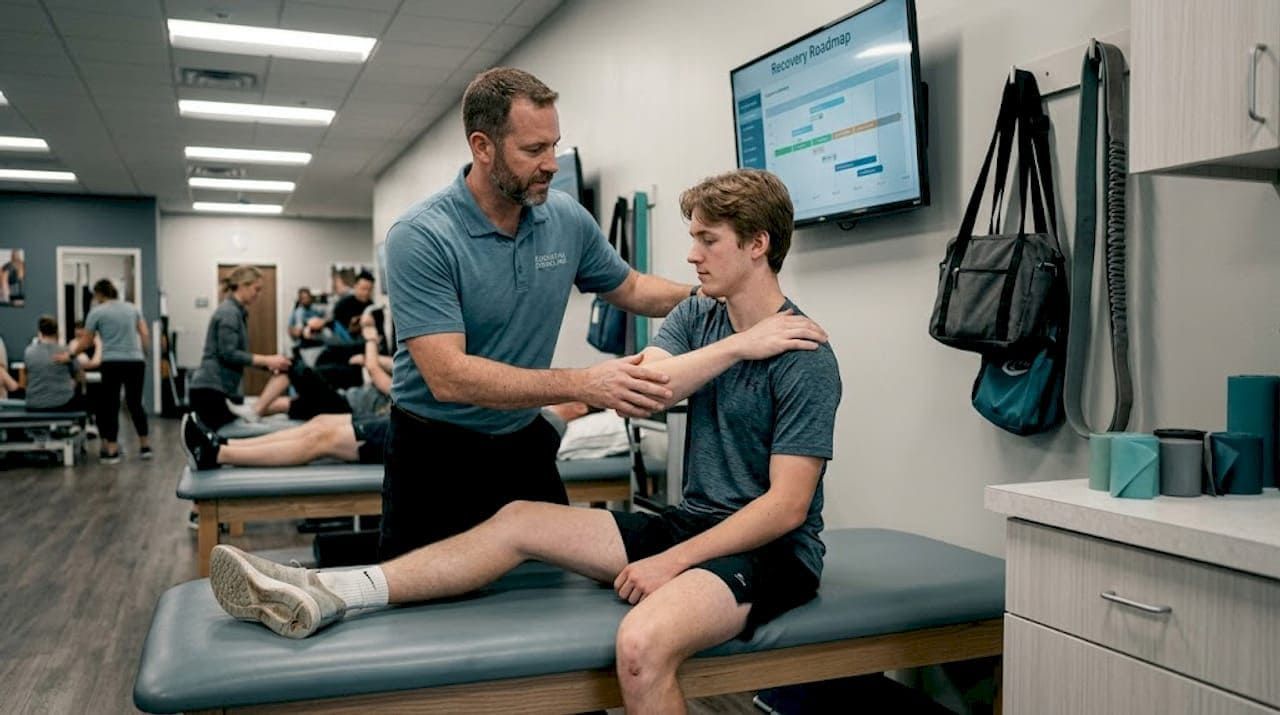
Step 4: Achieving lasting results and preventing reinjury
Following successful treatment, it is critical to turn your gains into lasting improvement and avoid future injuries.
Graduating from active treatment is a milestone worth celebrating, but it is not the end of the workflow. The habits and strategies you build during recovery become your long-term defense against reinjury. Clinics focus on long-term function with prevention and wellness, and the smartest patients carry that mindset home with them.
Returning to sports or daily activity should be gradual and deliberate. A good rule of thumb is the 10% rule: increase your activity load by no more than 10% per week. This gives connective tissue time to adapt without getting overwhelmed. Your provider will help you map out a return-to-activity timeline that fits your specific injury and lifestyle.
Here are simple daily habits that protect your progress:
- Warm up before any physical activity, even a walk around the block
- Stretch the muscle groups that were involved in your injury every morning
- Strengthen your core consistently, since it supports every movement your body makes
- Stay hydrated, because dehydrated tissue is more prone to strain
- Sleep seven to nine hours per night, since most tissue repair happens during deep sleep
- Avoid sitting or standing in one position for more than 45 minutes at a stretch
Re-injury prevention strategies also include periodic wellness visits, even after you feel fully recovered. Think of these like oil changes for your body. They catch small alignment issues, muscle imbalances, or movement compensations before they snowball into a new injury.
Pro Tip: Start a simple recovery journal. Write down one small win every day, whether it is less morning stiffness, a longer walk, or a better night's sleep. This practice keeps your motivation high and gives you and your provider a clear record of your progress over time.
Why most people underestimate the power of a structured recovery workflow
With your workflow complete, let's reflect on why every step actually matters and what most people miss.
Here is the uncomfortable truth: most people treat injury recovery like a light switch. Pain on, treatment starts. Pain off, treatment stops. That approach feels logical, but it ignores how the body actually heals. Tissue repair, neuromuscular retraining, and movement pattern correction all happen on timelines that run longer than pain relief. Stopping care when symptoms fade is like stopping antibiotics when you feel better. The underlying problem is still there.
In our clinical experience, patients who skip the assessment phase often spend weeks on treatments that do not match their actual injury. And patients who end care at the first sign of improvement are the ones we see again six months later with the same problem, usually worse. The workflow is not bureaucracy. It is biology made practical.
There is also a mindset issue worth naming. Many patients treat each appointment as a passive experience, something that happens to them rather than something they actively participate in. But the workflow only works when you engage with it. That means doing your home exercises, tracking your symptoms honestly, and communicating changes to your care team without waiting to be asked.
The patients who recover strongest and fastest are not always the ones with the least severe injuries. They are the ones who treat every step of the workflow as non-negotiable. Assessment, personalized planning, consistent treatment, honest progress tracking, and prevention are not optional extras. They are the actual shortcut. Skipping steps to save time almost always costs more time in the end.
For athletes especially, injury recovery for athletes requires this same disciplined approach, because the demands placed on a recovered body are higher than for the average patient. The workflow scales to meet those demands when you commit to every phase.
Take the next step in your recovery with expert help
Ready to put your workflow into action? Local experts can guide you through every step.
A personalized, clinic-guided recovery workflow is not just a nice idea. It is the difference between partial recovery and full function. At Essential ChiroCare, our team works with you from day one to build a plan that fits your injury, your goals, and your life in West Central Florida.
Whether you are dealing with a sports injury, an auto accident, chronic back pain, or a nagging joint problem, our chiropractic care services and rehab services are designed to move you through every stage of the workflow with precision and care. If spinal issues are part of your picture, our spinal decompression guide explains exactly how that therapy fits into a broader recovery plan. Reach out today to schedule your initial assessment and take the first real step toward lasting recovery.
Frequently asked questions
What is the most important step in an injury recovery workflow?
The most important step is the initial assessment, which guides personalized treatment and sets realistic goals. Personalization via assessments and tracking ensures tailored care that produces better results than generic protocols.
How often should progress be checked during recovery?
Progress should be reviewed at each chiropractic visit, typically weekly or biweekly, so adjustments can be made promptly. Progress tracking improves both adherence and long-term outcomes.
Can a workflow help prevent injuries in the future?
Yes, following a structured workflow teaches you prevention techniques and reinforces lifelong healthy habits that reduce reinjury risk. Clinics focus on long-term function with prevention built into every phase of care.
Is nutrition part of an injury recovery workflow?
Yes, nutrition supports healing and is often included in personalized recovery plans alongside physical treatments. Nutrition aids performance and healing in ways that directly speed tissue repair and reduce inflammation.